Thailand struggles with chronic resistant malaria
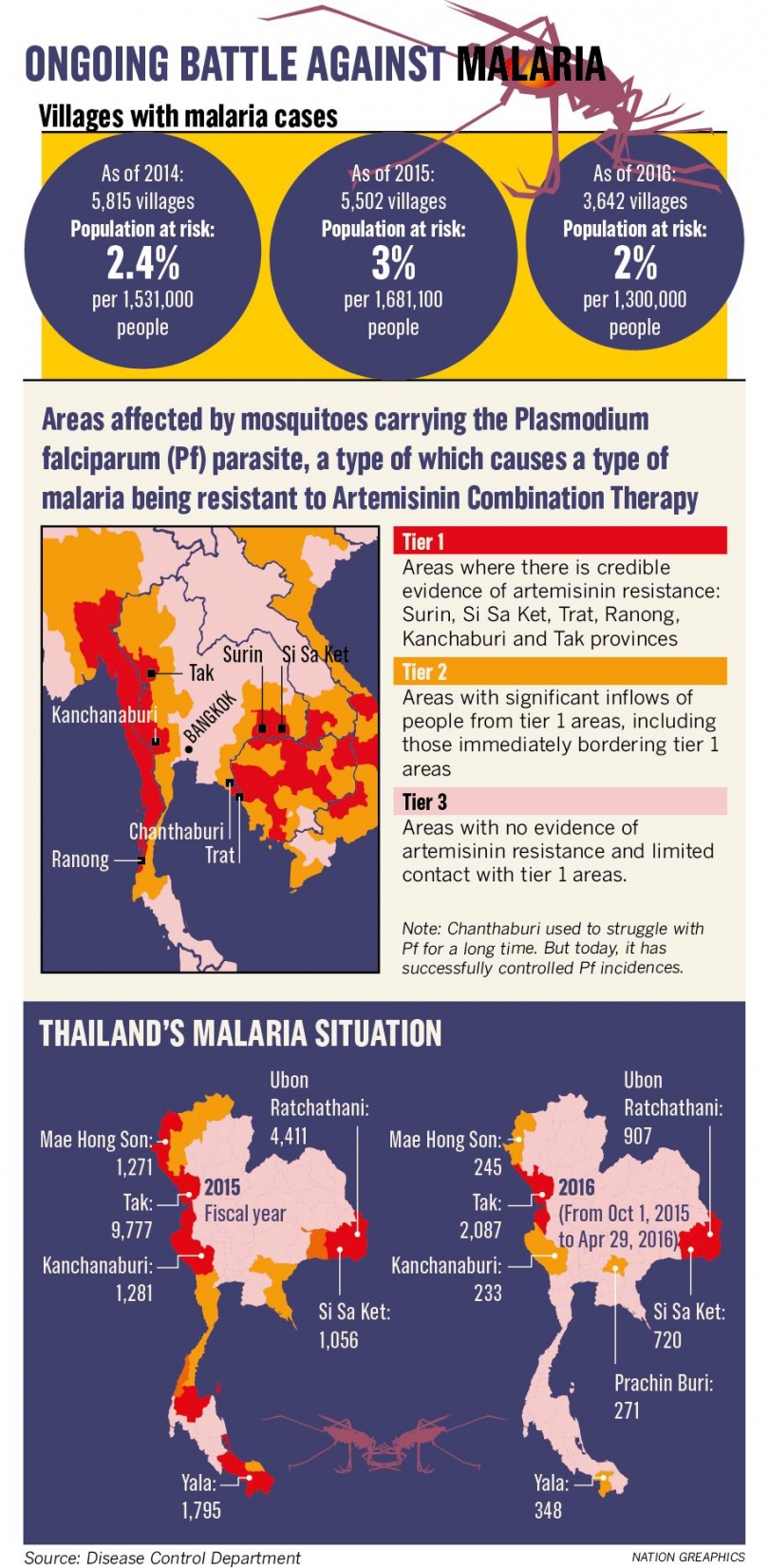
Three districts see recurrent pattern as drugs lose potency; 2024 eradication goal
THAILAND HAS a special spot on the global malaria map: It has always been the first territory to develop drug resistant new types of the disease.
Resistance to the anti-malarial drug chloroquine first emerged in Trat’s Bo Rai district and Chanthaburi’s Pong Nam Ron and Soi Dao districts many years ago.
A few years later, the resistance spread further to haunt two other affected provinces. After another few years had passed, it was a national threat.
“Then after a few more years, such drug resistance became widespread across the world,” said Dr Prayuth Sudathip, director of the Vector Borne Diseases Bureau.
He pointed out the pattern repeated itself after the arrival of newer medicines such as fansidar and mefloquine – with resistance starting in the same three original districts.
“After five or six years of mefloquine usage, we detected resistance in the same old areas. And soon, the resistance spread to other parts of the world as well,” Prayuth said.
According to Prayuth, artesunate was then recommended to replace mefloquine to control resistant types. More ingredients were later mixed with artesunate to produce a process now known as Artemisinin Combination Therapies (ACT) to try to prevent drug resistance from developing again.
“In 2008, we detected resistance against ACT in the small districts of Bo Rai, Pong Nam Ron and Soi Dao,” Prayuth said. “By 2010, the resistance had spread to Cambodia and Myanmar too.”
Prayuth said global healthcare professionals had seriously worked to rein in resistance to ACT because it was the most effective therapy to date.
“The best way was to eradicate malaria from drug-resistant areas like Thailand,” Prayuth said.
The Global Fund to Fight AIDS, Tuberculosis and Malaria gave US$100million (Bt3.5 billion) to Thailand, Myanmar, Laos, Cambodia and Vietnam for use between 2013 and 2016 to end resistance to malaria drugs.
“Myanmar received the biggest share. As for Thailand, we have received $10million,” he said.
Prayuth added that drug resistance had arisen with the Plasmodium falciparum (Pf) parasite due to three main factors: Genetics, failure to complete prescribed dosages and consumption of substandard medicines.
“We have found that substandard antimalarial medicines are quite common in our neighbouring countries. When patients take these poor-quality [drugs], they develop resistance to ACT. In the end, they might die because of malaria,” he said.
Researchers from the Paris-affiliated Institut Pasteur in Cambodia have found evidence that resistance to artemisinin in five countries of the Greater Mekong Subregion is also related to genetics. But once resistance starts, it can spread to other areas too, as seen in its expansion to India.
Efforts are now being made to stem the spread of resistant malaria once and for all. Otherwise, if these parasites reach regions where malaria is rife, such as areas in Africa, casualties would soar. Even now, when ACT remains effective, African countries still see hundreds of people succumbing to malaria each year.
Malaria is a mosquito-borne infectious disease caused by parasitic protozoan parasites belonging to the Plasmodium genus affecting humans and other animals.
People with malaria usually experience fever, chills and flu-like illnesses, which left untreated can lead to severe complications and death. In 2015, an estimated 214 million cases of malaria occurred worldwide and 438,000 people died, most of whom were children in Africa.
Prayuth said Thailand ranked among the countries that have had success fighting the disease, despite drug resistance problems.
The number of malaria patients in Thailand fell to just 24,000 last year, down by about 85 per cent from 150,000 in 2000.
“But we aim higher. We plan to make sure Thailand is free of malaria transmissions by 2024,” Prayuth said.
At present, malaria cases have been detected mostly in border provinces such as Ubon Ratchathani and Tak.
“Of all cases, just 30 per cent [of infected people] have caught the disease while in Thailand,” Prayuth said, pointing out that many patients were Karen and other Myanmar people.
The Greater Mekong Subregion as a whole plans to eradicate malaria completely by 2035.
Dr Rungrawee Tipmontree, who is also from the Vector Borne Diseases Bureau, said countries had to work together to control the disease.
“With the migration of peoples across borders, we need to join hands,” she said.
According to Rungrawee, volunteers have been used to educate people in risky zones about malaria symptoms and treatment.
“We need to reinforce the key message – if you live in areas with malaria threats, you get bitten by mosquitoes and develop fever, you should undergo blood tests to determine if you have malaria. That way, you will get proper diagnosis and treatment,” she said.
The Global Fund to Fight AIDS, Tuberculosis and Malaria has provided a budget for 140 countries across the world, including Thailand, in its bid to control malaria and fight drug resistance.
In Thailand, the budget is given to the Disease Control Department, which plans to complete a five-year project to fight the disease in September.
RELATED
